CABG vs. Angioplasty: How Do You Know Which One You Actually Need?
If you or someone in your family has been told that the heart arteries are blocked, the next conversation with your doctor often involves two words: bypass or angioplasty. Both are common. Both are well-established. And yet, for most patients, the difference between them is not entirely clear.
That confusion is understandable. The names sound technical, the decisions feel confusing, and every family member seems to have a different opinion pulled from somewhere on the internet.
Recognising when CABG or angioplasty is appropriate matters, as each approach addresses different patterns of coronary artery disease and impacts long-term outcomes differently.
Request a Consultation
What Is Coronary Angioplasty?
Coronary angioplasty, medically referred to as Percutaneous Coronary Intervention or PCI, is a procedure designed to open a blocked or narrowed coronary artery without open-heart surgery.
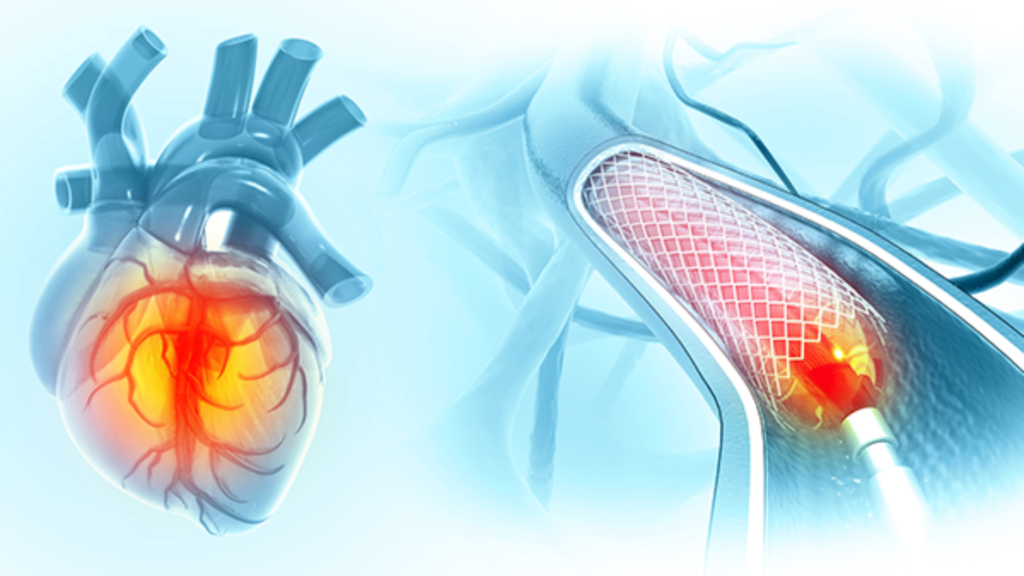
During the procedure, a thin, flexible tube called a catheter is inserted through the wrist or groin and guided to the blocked artery. A small balloon at the tip is inflated to widen the artery, and in most cases, a small metal mesh tube called a stent is left in place to keep the artery open.
The procedure typically takes one to two hours. Recovery is relatively quick. Most patients are discharged within a day or two.
What Is CABG Surgery?
CABG, which stands for Coronary Artery Bypass Grafting, is an open-heart surgical procedure.
A healthy blood vessel, usually taken from the leg, chest wall, or arm, is used to create a new pathway around the blocked artery. The blood can then bypass the blockage entirely and reach the heart muscle through this new route.
CABG requires general anaesthesia, a longer stay in hospital, and a recovery period that typically spans several weeks. It is a more complex undertaking, but in specific situations, it offers results that angioplasty simply cannot match.
Bypass Surgery vs Angioplasty: Which Treatment Is Right for You?
This is the most common question patients ask, and it is also the one that has no universal answer.
As Dr. Dinesh Kumar Mittal explains, “The question is never which procedure is better in general. The right question is which procedure is better for this particular patient, at this particular point in their disease. The anatomy of the blockage, the number of vessels involved, and the overall function of the heart all drive that decision.”
Neither procedure is superior on its own. Each has a clearly defined role depending on the nature and extent of coronary artery disease. For many patients, the decision becomes clearer only after they understand their own angiography in detail.
One patient described this moment of clarity: “I thought I would just need a stent because I had seen others recover quickly after angioplasty. But when my reports came, the doctor explained where the blockages were and why a stent wouldn’t be enough for me. It was not an easy decision, but once I understood the reason, I felt more comfortable going ahead with bypass surgery.”
Factors That Help Doctors Decide Between CABG and Angioplasty
1. Number of Blocked Arteries
If one artery is blocked and the blockage is suitable, angioplasty is often the preferred approach. It is less invasive, recovery is faster, and the outcomes are comparable in single-vessel disease.
When two or three major coronary arteries are significantly blocked, the balance shifts towards CABG. Multiple stents placed in multiple vessels can be done, but the long-term durability of bypass surgery in complex, multi-vessel disease has consistently shown better outcomes in clinical evidence.
2. The Left Main Artery
The left main coronary artery supplies a large portion of the heart muscle. When this artery is substantially blocked, most cardiac surgeons and cardiologists recommend CABG. The long-term data on bypass for left main disease have historically been strong, although angioplasty has become an option in carefully selected cases.
3. Diabetes
Patients with diabetes and multi-vessel coronary artery disease tend to do better with CABG in the long term. The FREEDOM trial, a large clinical study, found that bypass surgery reduced the risk of heart attack and death more effectively than stenting in diabetic patients with multi-vessel disease. This is now factored into international guidelines.
4. The Complexity of the Blockage
Not all blockages are equal. Some are short and accessible. Others are long, calcified, located at vessel junctions, or involve total occlusions. Angioplasty works well for straightforward lesions. When the anatomy is complex, forcing a stent through a difficult blockage carries a higher procedural risk, and the durability of the result may be less predictable. In those situations, a surgeon’s hands often produce a more reliable repair.
The nature of the blockage often changes the direction of treatment more than initial expectations. As one patient shared: “I was hoping for angioplasty because it seemed simpler. But when the doctors explained that the blockage was heavily calcified and not ideal for a stent, it made sense why surgery was being recommended. What helped was that they didn’t rush the decision; they made sure I understood it.”
5. Heart Function
If the heart muscle has been weakened, perhaps from a previous heart attack, the overall pumping function matters. Patients with significantly reduced ejection fraction may benefit from the more complete revascularisation that bypass surgery can provide.
When Is Angioplasty Preferred in Coronary Artery Disease?
Angioplasty is typically recommended when the disease pattern allows for a safe, durable stent placement. It tends to be the preferred option when:
- There is a single significant blockage in one vessel
- A patient is having an acute heart attack, and the artery needs to be opened immediately
- A patient is not fit enough to undergo open-heart surgery due to other health conditions
- The blockage is anatomically straightforward and in a location that responds well to stenting
In an emergency such as an acute heart attack, angioplasty is almost always done first. Speed matters, and the catheter lab can be reached faster than a theatre can be prepared for surgery.
When Does CABG Surgery Offer Better Long-Term Outcomes?
CABG is generally advised when coronary artery disease is more extensive or complex, where a more complete and durable restoration of blood flow is required. It is the preferred option when:
- Three major vessels are significantly blocked (triple vessel disease)
- The left main coronary artery is involved
- The patient has diabetes alongside complex multi-vessel disease
- The coronary anatomy is too complex for reliable stenting
- Repeat procedures are needed after stents have re-narrowed (a problem called in-stent restenosis)
Dr. Dinesh Kumar Mittal notes, “Bypass surgery gives the heart new highways. When the disease is extensive, those new routes provide far more complete protection than stents can in many cases. It is a bigger operation with a longer recovery, but for the right patient, the long-term benefit is worth it.”
CABG vs Angioplasty: Recovery and Long-Term Outlook
Recovery timelines differ, but so do long-term outcomes. Angioplasty offers quicker recovery, while CABG may provide more durable results in selected patients.
After Angioplasty (Stenting)
- Most patients are discharged within 24 hours
- Mild soreness at the catheter entry site is common
- Normal daily activity usually resumes within a week
- Many patients return to work within 1-2 weeks
- Requires dual antiplatelet medication (blood thinners) for a prescribed duration
After Bypass Surgery (CABG)
- Hospital stay is typically 5-7 days
- Initial recovery at home takes 2-4 weeks with limited activity
- Most patients resume routine activities, including driving, by around 6 weeks
- Cardiac rehabilitation is strongly recommended for better long-term recovery
Long-Term Considerations (For Both)
Long-term outcomes depend on:
- Heart-healthy diet
- Regular physical activity
- Stopping smoking
- Control of blood pressure, cholesterol, and blood sugar
- Consistent medication adherence
As Dr. Dinesh Kumar Mittal explains, “Recovery is not just about how quickly you get back to normal, but how well the treatment supports your heart health over the years. That is what ultimately guides the choice between procedures.”
CABG vs Angioplasty: Understanding the Risks
No procedure is without risk, and understanding this is important in making the right decision.
| Aspect | Angioplasty (Stenting) | Bypass Surgery (CABG) |
|---|---|---|
| Type of Procedure | Minimally invasive (catheter-based) | Open-heart surgery |
| Short-Term Risk | Lower immediate risk | Higher due to major surgery |
| Common Risks | Re-narrowing of the artery (restenosis)
Blood clot in the stent Bleeding at the insertion site |
Infection at the surgical site
Bleeding or need for transfusion Stroke (rare) |
| Long-Term Considerations | May require repeat procedures in some cases | More durable in complex or multi-vessel disease |
| Recovery | Faster recovery, shorter hospital stay | Longer recovery and hospital stay |
Understanding these risks helps put the decision in perspective, not just in terms of the procedure itself, but in terms of what it means for long-term heart health.
As Dr. Dinesh Kumar Mittal explains, “Every treatment option has its own set of risks. The key is to weigh those risks against the expected long-term benefit. In many cases, what seems like the simpler option upfront may not always provide the most durable outcome.”
Should You Seek a Second Opinion?
For any major cardiac intervention, especially when CABG is being considered, a second opinion is not only reasonable but also recommended.
A meaningful consultation should focus on your angiography findings, disease pattern, and long-term risk, not just general comparisons between procedures.
If you are considering CABG or angioplasty in Delhi, consulting an experienced surgeon like Dr Dinesh Kumar Mittal can help clarify the most appropriate treatment plan based on your specific condition.
The Right Procedure Is the One Your Heart Actually Needs
Angioplasty and bypass surgery are not competing options. They solve different problems. One is not braver or better than the other.
What drives the decision is your coronary anatomy: how many arteries are blocked, how complex those blockages are, whether diabetes is in the picture, and how well your heart is currently functioning. That is information only an angiography and an experienced cardiac surgeon can properly interpret.
As Dr. Dinesh Kumar Mittal says, “A good recommendation is not about what is easier to perform or easier to hear. It is about what your specific coronary anatomy demands.”
If you have been diagnosed with coronary artery disease and are weighing your treatment options, the next step is a detailed consultation with a specialist who will look at your case, not a general statistic.

